We use cookies on this site to improve our service, perform analytics, and remember website preferences. By using this site, you consent to these cookies. For more information visit our Privacy Policy
Changing pain management for youth undergoing surgery
HHF collaborated with Partnering for Pain, a patient oriented research program, to better understand the lived experience of youth with chronic post-surgical pain and to design a service where their pain could be better supported and managed. Partnering with youths, family members, health leaders and decision makers allowed us to envision our ideal potential future state and design with that in mind.
In Collaboration With
Partnering for Pain
University of Calgary
Services
Service design, co-design workshops
Challenge
In pediatric settings, Chronic Postsurgical Pain (CPSP) is experienced all too often without proper resources in place to appropriately support youth and their families. Every year, approximately 80,000 Canadian children undergo surgery and about 20% who undergo major surgery will develop CPSP. Under treatment or poor management of pain prior to and following surgery is widespread and can lead youths to feel anxious, have difficulty sleeping, and develop problems socially and at school. These challenges affect both the youth and their family, and could be prevented if there were services in place to better manage post-operative pain and prevent it from becoming chronic.
To better serve youth and families we wanted to build on, and refine, existing Pediatric Transitional Pain services to create a service model that could be implemented at any healthcare organization.
When you see your child in that much pain and there’s nothing you can do, it’s just so disheartening.
Parent
Process
Discovery
We began by immersing ourselves in interview transcripts that the Partnering for Pain team had conducted with youth, families and healthcare professionals to gain an initial understanding of the lived experience.
We then held two co-design workshops with youth, families, healthcare professionals, and decision makers to begin unpacking what the ideal experience would be to prevent and manage pain along the continuum of care.
By understanding the ideal experience, we were able to glean key insights that would remain the keystones of our service design.
What We Discovered
Partnerships are Key
To enable youth and families to self advocate, a true partnership is required with healthcare professionals. Engaging with youth and families holistically would provide opportunities to collaboratively develop personalized care plans to prevent and manage pain.
Leave No Youth Behind
All youth being referred to surgical specialty clinics should be screened to assess if they would benefit from this service. This ensures that risk factors for CPSP can be readily identified for prevention and/or early intervention.
Prioritize and Give Pain a Home
Currently there is a disconnect between surgical disciplines and pain prevention and management. They are seen as distinct teams with separate purposes. Better integration and governance would allow for the gap to be bridged and for pain to truly have a home within the circle of care.
Outcomes
The co-design process culminated in a service delivery model, the Surgical Integrated Pain Service (SIPS). Informed by, and designed for youth and families, SIPS gives pain a home for youth undergoing surgery. It keeps conversations about pain at the centre, champions proactive and comprehensive pain management, and allows for a personalized experience across the continuum of care. The service model is illustrated in an interactive service blueprint. While designed for medium to high resourced organizations, throughout the blueprint there are insights and considerations that provide recommendations for how to modify the SIPS model to meet resource constraints.
We need to acknowledge and strengthen youth and listen to their needs, considering multiple strategies extending beyond medications
Healthcare Professional

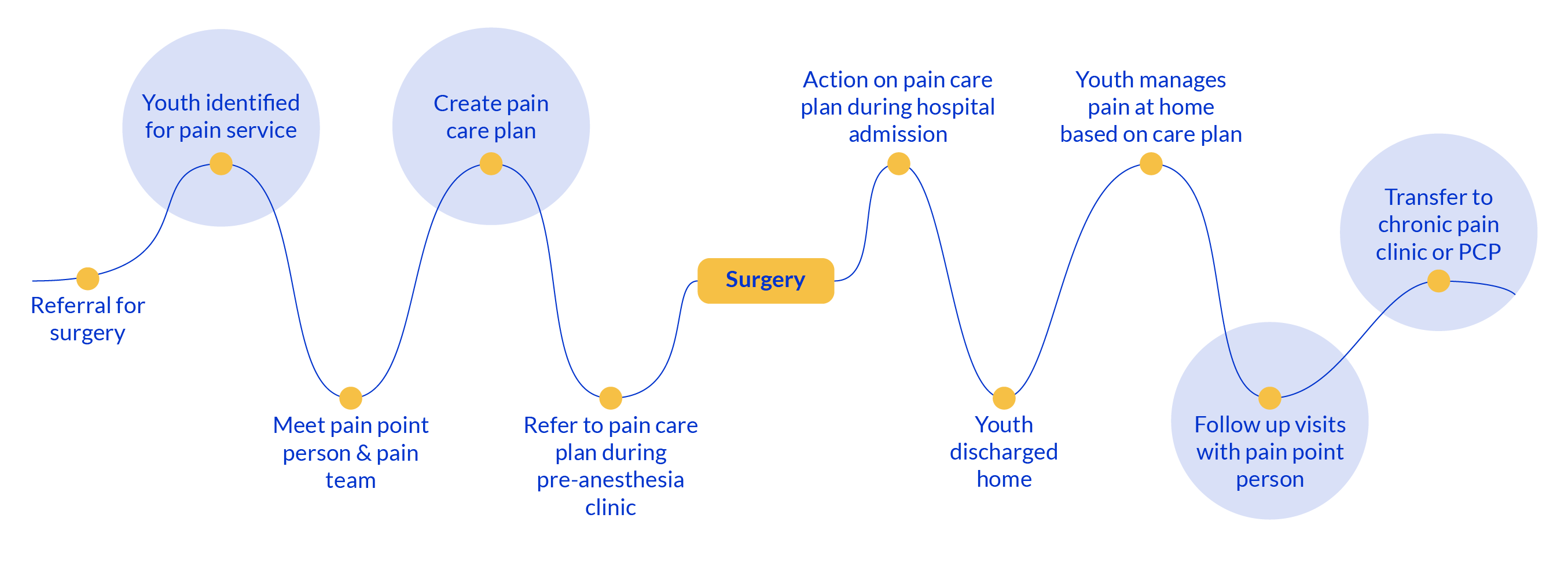
Informed by, and designed for youth and families, the Surgical Integrated Pain Service (SIPS) gives pain a home.